Collaborative Care (CoCM) is a specific type of integrated care developed at the University of Washington to treat common mental health conditions in medical settings like primary care. Behavioral health conditions such as depression, anxiety, PTSD, alcohol or substance use disorders are among the most common and disabling health conditions worldwide. Based on principles of effective chronic illness care, CoCM focuses on defined patient populations who are tracked in a registry to monitor treatment progression. The treatment plan focuses on measurement-based treatment to target, to ensure the patient’s goals and clinical outcomes are met.
Collaborative Care Team
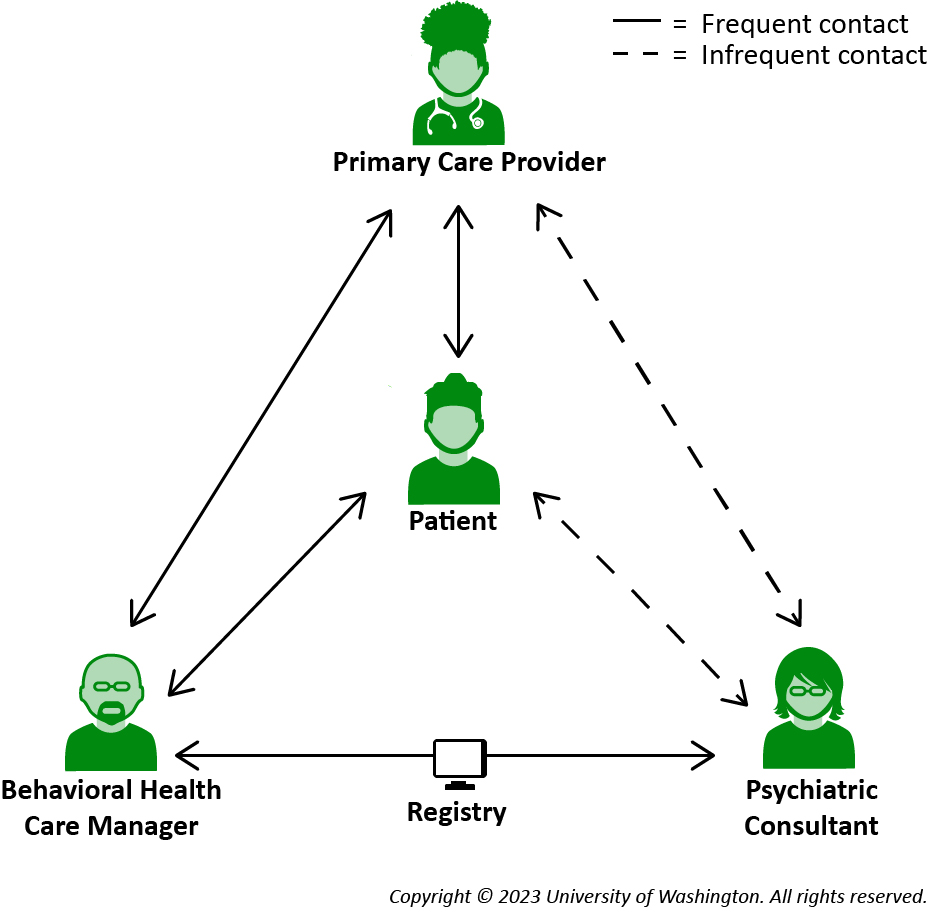
CoCM requires a team of providers. Trained Primary Care Providers (PCP) work with embedded Behavioral Health Care Managers (BHCM) to provide evidence-based medication or psychosocial treatments. The PCP and BHCM are supported by a Psychiatric Consultant who meets regularly with the BHCM for Systematic Caseload Review (SCR), where they consult on patients and adjusts treatment for those who are not improving as expected.
Collaborative Care Outcomes
CoCM has now been tested in more than 90 randomized controlled trials in the US and abroad, and is widely agreed upon as the integrated care approach with the most robust evidence base. It leads to significantly better clinical outcomes, greater patient and provider satisfaction, improved functioning, and reduces health care costs. Collaborative Care necessitates a practice change on multiple levels and is nothing short of a new way to practice medicine, but it works. The bottom line is that providers have the resources they need to most effectively treat patients and the patients are twice as likely to get better in significantly less time (86 days vs. 614 days in usual care).
The video below is also available with audio description.
Resources
Use our Resource Library to find materials about Collaborative Care, have our Implementation Guide take you through the process of implementation, or browse the following pages to better understand the model.